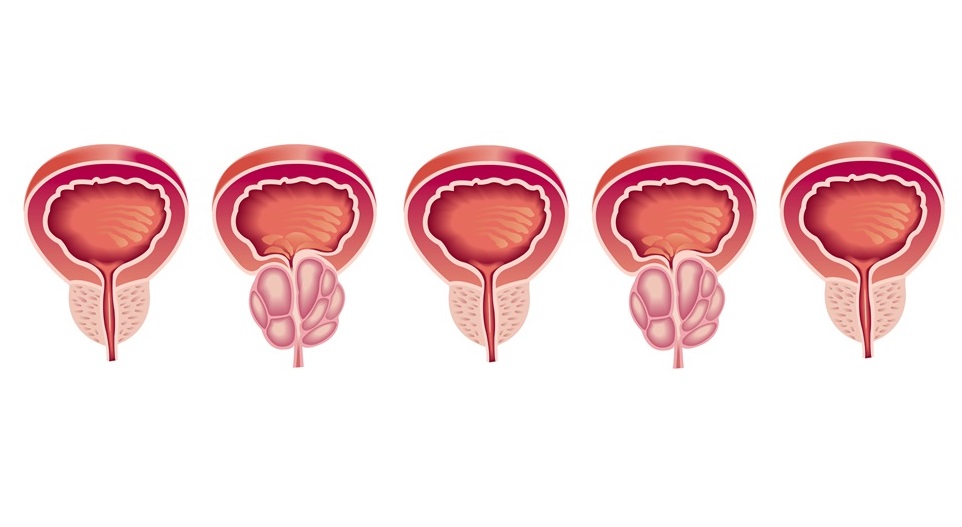
For prostate cancer sufferers, the PSA test and Gleason score may be on their way out as a new landmark study has shown superior ability to predict which of the 5 prostate cancers — also a new development — are likely to be most aggressive.
Researchers at Cancer Research UK Cambridge Institute and Addenbrooke’s Hospital analyzed tissue samples from over 250 men and found that they could group the diseased cells into five distinct types. Each of the abnormal cell types had a characteristic genetic pattern.
“Our exciting results show that prostate cancer can be classified into five genetically-different types,” study author Dr Alastair Lamb said of the work. “These findings could help doctors decide on the best course of treatment for each individual patient, based on the characteristics of their tumour.
Although the proceedure needs to be confirmed with larger trials, in its initial phases it has shown itself more effective than the current prostate cancer tests, the PSA test and Gleason score, according to the researchers.
“The next step is to confirm these results in bigger studies and drill down into the molecular ‘nuts and bolts’ of each specific prostate cancer type,” Lamb said. “By carrying out more research into how the different diseases behave we might be able to develop more effective ways to treat prostate cancer patients in the future, saving more lives.”
Because the tumors of the five types may be better dealt with based on their type, the research could significantly improve prostate cancer treatments. This is particularly important, Dr. Malcolm Mason, Cancer Research UK’s prostate cancer expert, noted, because prostate cancer varies widely in the way it develops: sometimes it grows slowly and may not cause problems in a man’s life; other times it spreads aggressively and demands immediate treatment.
“The challenge in treating prostate cancer is that it can either behave like a pussycat — growing slowly and unlikely to cause problems in a man’s lifetime — or a tiger — spreading aggressively and requiring urgent treatment, noted Mason. “But at the moment we have no reliable way to distinguish them. This means that some men may get treatment they don’t need, causing unnecessary side effects, while others might benefit from more intensive treatment.
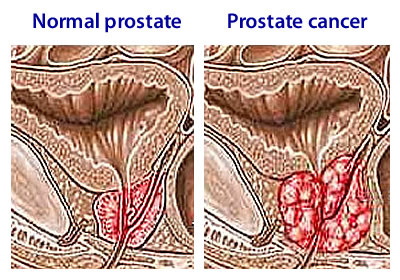
“This research could be game-changing if the results hold up in larger clinical trials and could give us better information to guide each man’s treatment — even helping us to choose between treatments for men with aggressive cancers. Ultimately this could mean more effective treatment for the men who need it, helping to save more lives and improve the quality of life for many thousands of men with prostate cancer.”
By Cheryl Bretton